Recent market research has shown a worldwide increase in the use of prostheses and orthoses, primarily driven by the increasing prevalence of diabetes in both children and older people.
These mobility assistive devices are designed to either artificially replace a lost limb or body part, or provide additional support to enable easier movement.
Because these devices are directly in contact with the user’s skin for long periods of time – particularly the inner sides of prosthetic sockets and orthotic devices – there is a clear need to help manage the levels of the potential foreign microorganisms present and limit any risk of infection to the user from harmful bacteria, fungi or viruses.
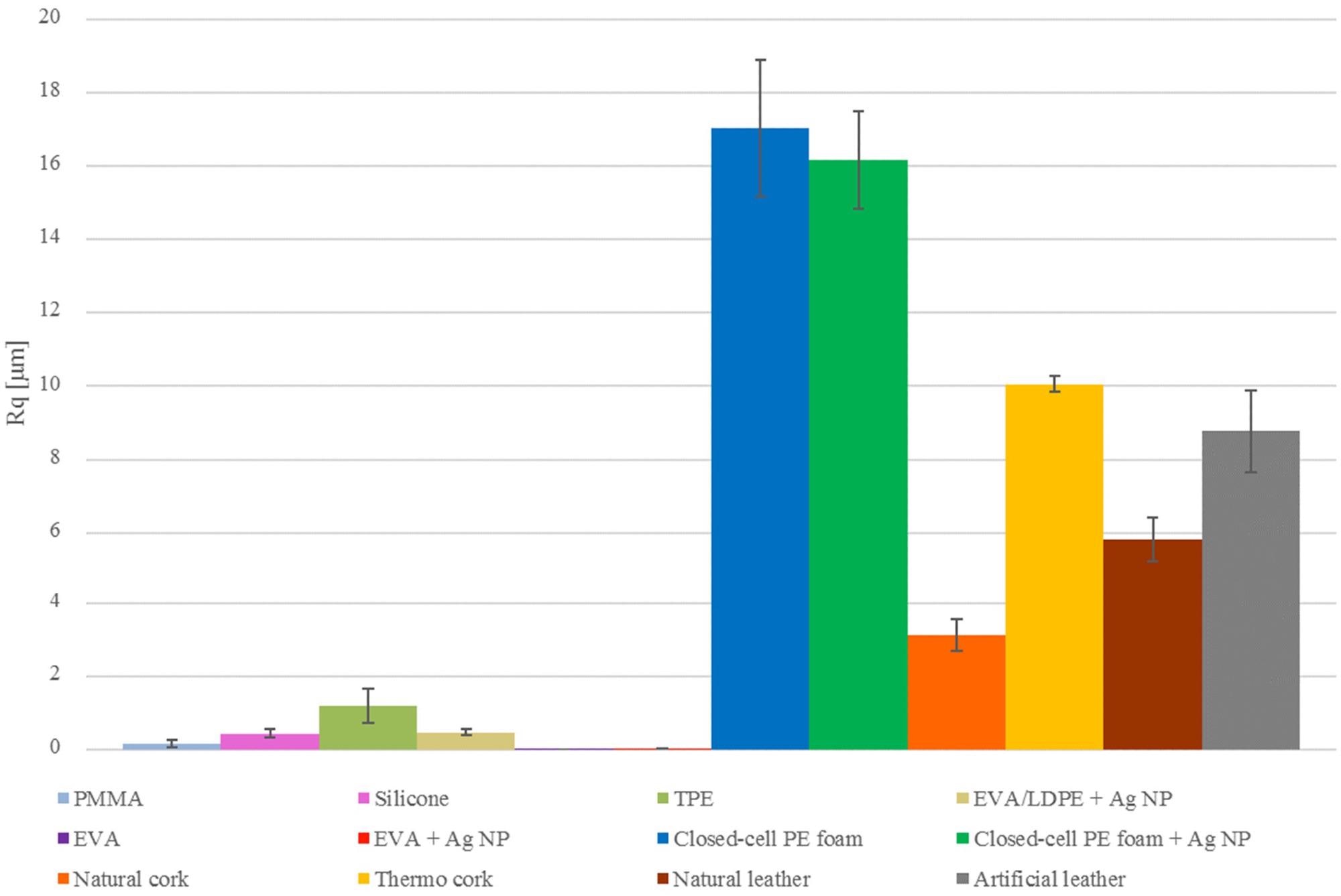
RMS roughness Rq of orthotic and prosthetic surfaces measured with the profilometer. Image Credit: Abram, A et al., Coatings
Bacteria such as staphylococcus (S.) aureus and S. epidermidis are almost constantly resident on a person’s skin, and there is a risk that some strains of these bacteria may adhere to prostheses and orthoses’ solid surfaces and develop biofilms which may, in turn, lead to infections when these are in contact with an impaired skin barrier.
This phenomenon of bacteria becoming firmly attached to surfaces is typically referred to as bacterial adhesion.
Research is ongoing into the factors which can affect bacterial adhesion, but these factors have already been found to include surface charge, surface hydrophobicity, and the material’s surface roughness.
A number of historic studies into bacterial adhesion to medical devices have looked into the adhesion of staphylococci bacteria to the materials used for implantable medical devices, but the paper’s authors report that they did not find any studies exploring the adhesion of bacteria to prosthetic and orthotic materials.
With this in mind, they aimed to demonstrate how the surface properties of different prosthetic and orthotic materials typically in contact with skin had the potential to impact the capacity and likelihood of S. aureus and S. epidermidis adhering onto the materials’ surface.
The authors evaluated the most commonly used materials for orthotic and prosthetic devices, investigating the materials’ capacity to attract the bacteria commonly present on the skin.
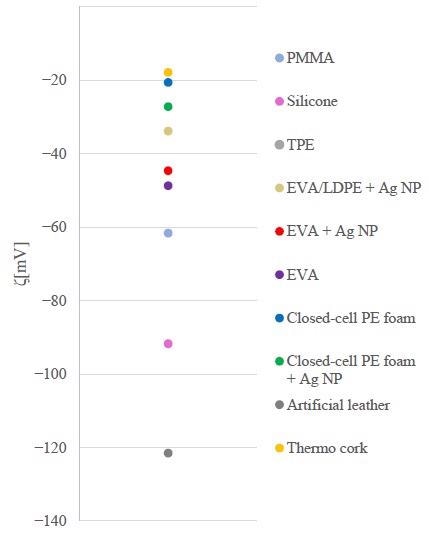
Zeta potentials of orthotic and prosthetic material surfaces. Image Credit: Abram, A et al., Coatings
This particular study was focused on the materials’ surface characteristics such as wetting, surface charge, roughness, and morphology.
Twelve different materials typically used in prosthetics and orthotics were evaluated, including two natural materials (natural leather and natural cork) and ten synthetic materials including ethylene-vinyl acetate (EVA), silicone, artificial leather, and poly(methyl methacrylate) (PMMA).
In order to look at a possible means of better mitigating this bacterial adhesion, the authors also evaluated the potential of silver nanoparticle coatings to affect the bacterial adhesion to materials – a novel approach, since almost all studies of S. aureus and S. epidermidis’ adhesion to material surfaces have historically focused on the titanium and titanium alloys employed in implants. To this end, three of the materials investigated included these coatings.
Bacteria with hydrophobic properties have been found to attach more robustly to the surfaces of similarly hydrophobic materials – more so than the adhesion of hydrophilic bacteria. Hydrophobic materials have been noted to be less resistant to bacterial adhesion than hydrophilic materials.
Surface roughness – for example, defects such as dimples, grooves, and cracks – has also been found to encourage bacterial adhesion and the development of biofilm.
Another factor that can impact the potential for bacterial adhesion is a surface charge. The majority of solid surfaces and bacteria are negatively charged and should bacteria and a material’s surface exhibit the same charge, repulsive electrostatic forces will cause an energy barrier that prevents adhesion.
SEM micrographs were used to evaluate the extent of bacterial adhesion, while data was acquired on a range of materials’ surface topographies, roughness, hydrophobicity, and zeta potential.
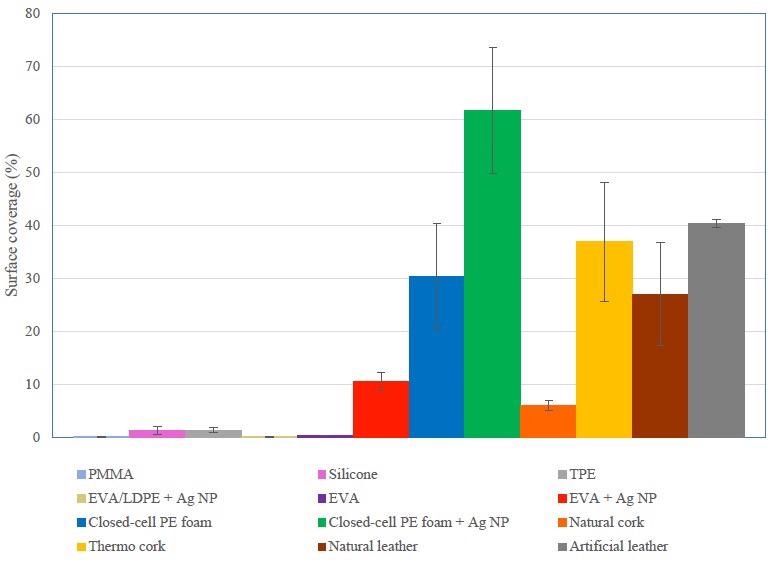
Surface coverage for different orthotic and prosthetic materials based on the evaluation of SEM micrographs. On the first four surfaces, S. epidermidis is adhered, whereas, on the rest of the surfaces, S. aureus adheres. Image Credit: Abram, A et al., Coatings
This study revealed that the most prominent bacterial adhesion existed on the analyzed artificial leather and thermo cork, while the least prominent bacterial adhesion was observed on the ethylene-vinyl acetate samples. The authors concluded that this material’s specific surface characteristics, such as roughness, hydrophobicity, and charge, were the key factors in this reduced bacterial adhesion.
By better understanding which orthotic and prosthetic materials are able to reduce bacterial adhesion when exposed to the bacteria found on the skin, manufacturers of these vital devices will be able to select materials that specifically reduce this.
This will ultimately reduce the risk of bacterial infection and help to protect users of prosthetics and orthotics more effectively.
References
Abram, Anže, Anamarija Zore, Urban Lipovž, Anita Košak, Maja Gavras, Žan Boltežar, and Klemen Bohinc. 2021. "Bacterial Adhesion on Prosthetic and Orthotic Material Surfaces" Coatings 11, no. 12: 1469. https://www.mdpi.com/2079-6412/11/12/1469
Cision. 2021. “Prosthetics Market worth $ 13.12 Billion, Globally, by 2028 at 4.51 %W https://www.prnewswire.com/news-releases/prosthetics-market-worth--13-12-billion-globally-by-2028-at-4-51--cagr-verified-market-research-301287440.html
Disclaimer: The views expressed here are those of the author expressed in their private capacity and do not necessarily represent the views of AZoM.com Limited T/A AZoNetwork the owner and operator of this website. This disclaimer forms part of the Terms and conditions of use of this website.