Wound healing is a crucial physiological process through which damaged tissues repair themselves. Chronic wounds considerably affect a patient’s quality of life, incur high treatment costs, and are associated with high mortality in diabetic and bedridden patients.
 A person’s leg wrapped in bandage (not the smart bandage from this research). Image Credit: Nutnaree Saingwongwattana/Shutterstock.com.
A person’s leg wrapped in bandage (not the smart bandage from this research). Image Credit: Nutnaree Saingwongwattana/Shutterstock.com.
Chronic wounds can be a cause of major suffering and disability for patients. Healing such wounds is tricky, and various factors can affect wound healing, for example, moisture level, pH, temperature, uric acid, lactate, and glucose levels, as well as infection status. If the wound is too dry, the tissue can become desiccated. If it is too wet, it can become white and wrinkly. Both these conditions disrupt the healing process.
The key to enabling chronic wounds to heal is to maintain optimal levels of moisture. At present, there is no way to check moisture levels without removing a bandage, which disrupts the healing process.
To this end, researchers have now developed a “smart bandage” that measures and wirelessly transmits wound moisture data in real-time, which could help treat chronic wounds.
Fabrication
The fabrication of the moisture sensor is a two-step procedure. First, the active material is deposited, and second, three different textile-based layers are assembled together to obtain a smart and sensitive wound dressing.
The moisture sensor is based on two electrodes of poly(3,4-ethylenedioxythiophene):polystyrene sulfonate (PEDOT:PSS) separated by a defined distance. The PEDOT:PSS was applied onto a gauze using screen printing and the gauze was incorporated with commercially available bandage materials.

Active gauze textile substrates. (A–B) Enlarged top view and (C–D) top view photos of the active substrates showing the different spreading of a colored liquid through the textile surface of PET and Rayon gauzes.
How the Smart Bandage Works
The new smart bandage includes a moisture sensor with the ability to measure wound moisture levels very sensitively and then transmit the data to a nearby smartphone, thereby avoiding the need to remove the bandage.
The concept behind the bandage is that changes in the moisture level of the wound lead to a change in an electrical signal measured by the sensor.
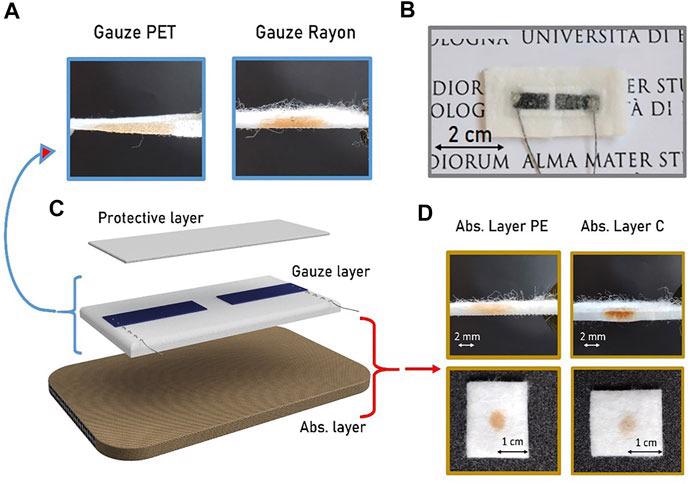
Complete moisture sensors architecture. (A) Cross section of the Gauzes PET and Rayon with the diffusion profile of a colored drop. (B) Optical image of the final textile moisture sensor prototype. (C) Structure of the bandage sensor showing the three different composition layers. (D) Cross section and top views of the two absorbing layers used as reservoir substrate highlighting their different wettability.
Performance
The main feature that influences the sensor response and behavior is the composition of the textile substrate. The saturation volume relies on the particular properties of the absorption layer. The sensor’s behavior is not only influenced by the absorption coefficient but also by the horizontal distribution of exudate through the textile.
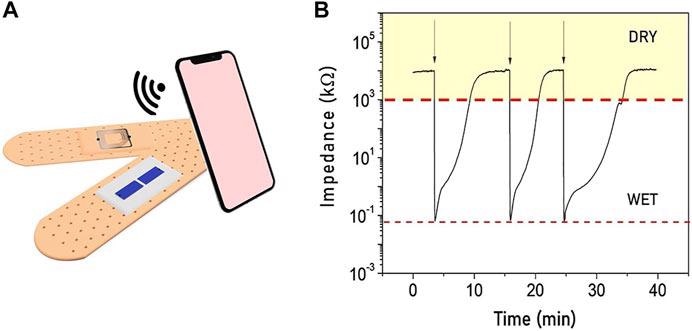
Illustration of the smart moisture bandage with the electrodes in the internal parts of the bandage and the RFID tamper alarm on the external side to realize a fully passive device. (B) Real-time monitoring of the sensor’s impedance when the status switches between wet and dry showing a reversible behavior.
The distance between the two printed conductive electrodes has a lower impact on the sensor performance. The large impedance variation of the sensor observed when it changes from being dry to wet enables it to be directly integrated with a passive RFID chip, thereby realizing an economical, passive, humidity sensor tag.
An ideal combination of gauze and absorption layer can help achieve an entirely passive smart bandage that can give an RFID tamper alarm when the wound switches from wet to dry and vice-versa.
Moreover, the moisture sensor includes a highly advanced RFID-NFC tag (NHS3152) to carry out quantitative measurements. The tag harnesses the RF signal and quantifies the sensor output connected between two of its terminals. Then, the measured value is read through a smartphone integrated with an NFC reader.
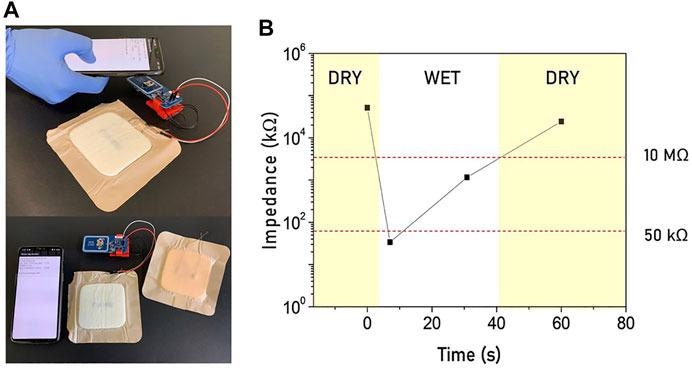
(A) Moisture sensor embedded in a real wound dressing and attached to an NFC interface. (B) The wireless communication with a NFC reader (a smartphone) allows to perform a quantitative measurement to investigate the wound condition in real-time.
The bandages were tested by exposing them to artificial wound exudate—the liquid that seeps from wounds. They were also tested with different bandage materials and shapes.
The bandage was found to be highly sensitive, offering considerably different readings between dry, moist, and saturated conditions. This suggests that it could be a valuable tool in wound management.
Results
A range of bandages with different layers and different absorption properties and characteristics were developed. It is possible to achieve tunable properties and performance based on the wound type.
The potential to connect the smart textile patch to an RFID and to an NFC interface results in a completely passive assembled smart bandage for fast, economical, disposable, and wireless real-time monitoring of wound moisture.
However, the sensor geometry will need to be further optimized and the appropriate sensor values for optimal healing will have to be determined before the technology can be applied to different types of wounds.
Journal Reference:
Tessarolo, M., et al. (2021) Wireless Textile Moisture Sensor for Wound Care. Frontiers in Physics. doi.org/10.3389/fphy.2021.722173.