Dentition loss, also known as edentulism, is one of the most serious oral health diseases. Although preventable, edentulism is nonetheless a frequent problem around the world. Dental implants became the standard therapy for whole or partial tooth loss in this context, replacing mobile dentures that are anchored in residual teeth or soft tissue and, as a result, shifted over time. Titanium implants are the most popular among the various materials available on the market because of their biocompatibility and low cost.
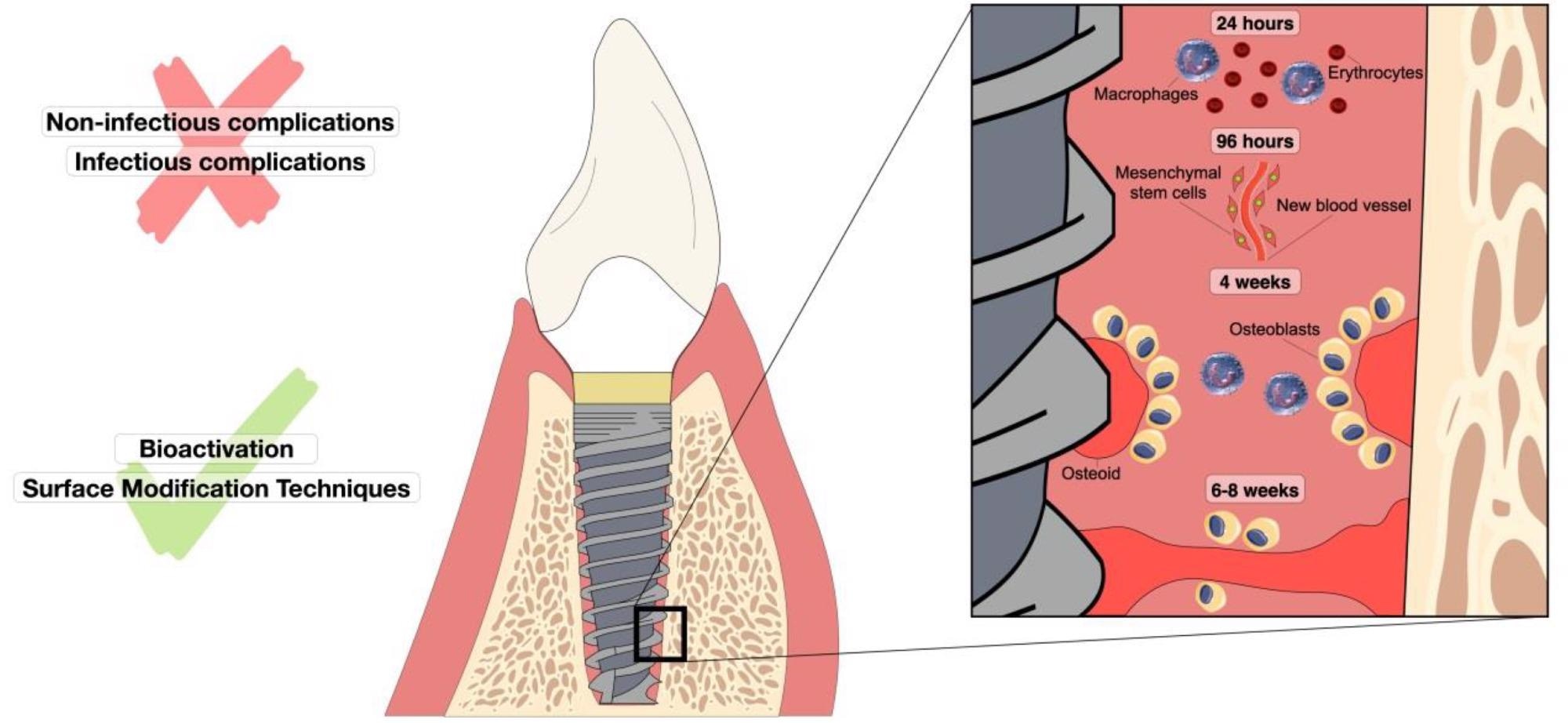
Representation of oral osseointegration events over time in a dental implant. The figure shows the sequence of cellular-level responses that occur after implant insertion for 24 h to approximately 8 weeks. Non-infectious and infectious complications are reported as factors that hinder osseointegration. Factors that improve this process are bioactivation and surface modification techniques. Image Credit: Silva, R. C. S et al., Materials
Despite the material's intrinsic advantages, it has a low level of integration with the bone and gingival tissue without proper surface treatment, which can lead to dental implant failures. Nanotechnology has had a favorable impact on dentistry, allowing for the creation of surfaces with a precise topography and chemical composition to increase material biocompatibility.
Surface bioactivation using biomolecules is also a hot topic of research to assure implant success in the long run. Biomolecules from the blood or created by the host tissue cells bind to the metal when it is implanted, allowing the cellular anchoring process to begin. As a result, bio-activating materials with biologically active chemicals can not only aid cell adherence, but also control their activity over the implant surface, stimulating cell migration, proliferation, and differentiation.
About the Study
In this study, the authors examined the various aspects of the use of titanium and its alloys in the manufacture of dental implants, as well as the most common reasons for implant failures and the development of better surfaces capable of promoting osseointegration and ensuring long-term implant success. Despite the fact that titanium could be used as the primary material in the creation of dental implants, several surface modifications were investigated in order to optimize the osseointegration process.
The researchers discussed the numerous factors that contribute to the effective osseointegration of titanium implants, as well as the most common surface treatments employed in the production of biomimetic surfaces for these implants. They presented an overview of various surface treatments that were researched for the development of high-performance titanium dental implants.
Observations
One of the studies looked at the use of the plasma electrolytic oxidation (PEO) treatment to create a biocompatible surface and improve osseointegration with in vitro and in vivo tests. The coatings were made for Ca/P ratios of 2.0 and 4.0, and both showed good cell adhesion and proliferation in murine osteoblasts, and the ratio of 1.8 showed improved bone-matrix mineralization.
The traditional process involved successive immersions in a mixture of sulfuric acid (H2SO4) and hydrochloric acid (HCl) solutions at a temperature of 50–70 °C, followed by surface cleaning. The highest success rate and quickest osseointegration time were found in mini hexagonal implants with a length of 4–6 mm.
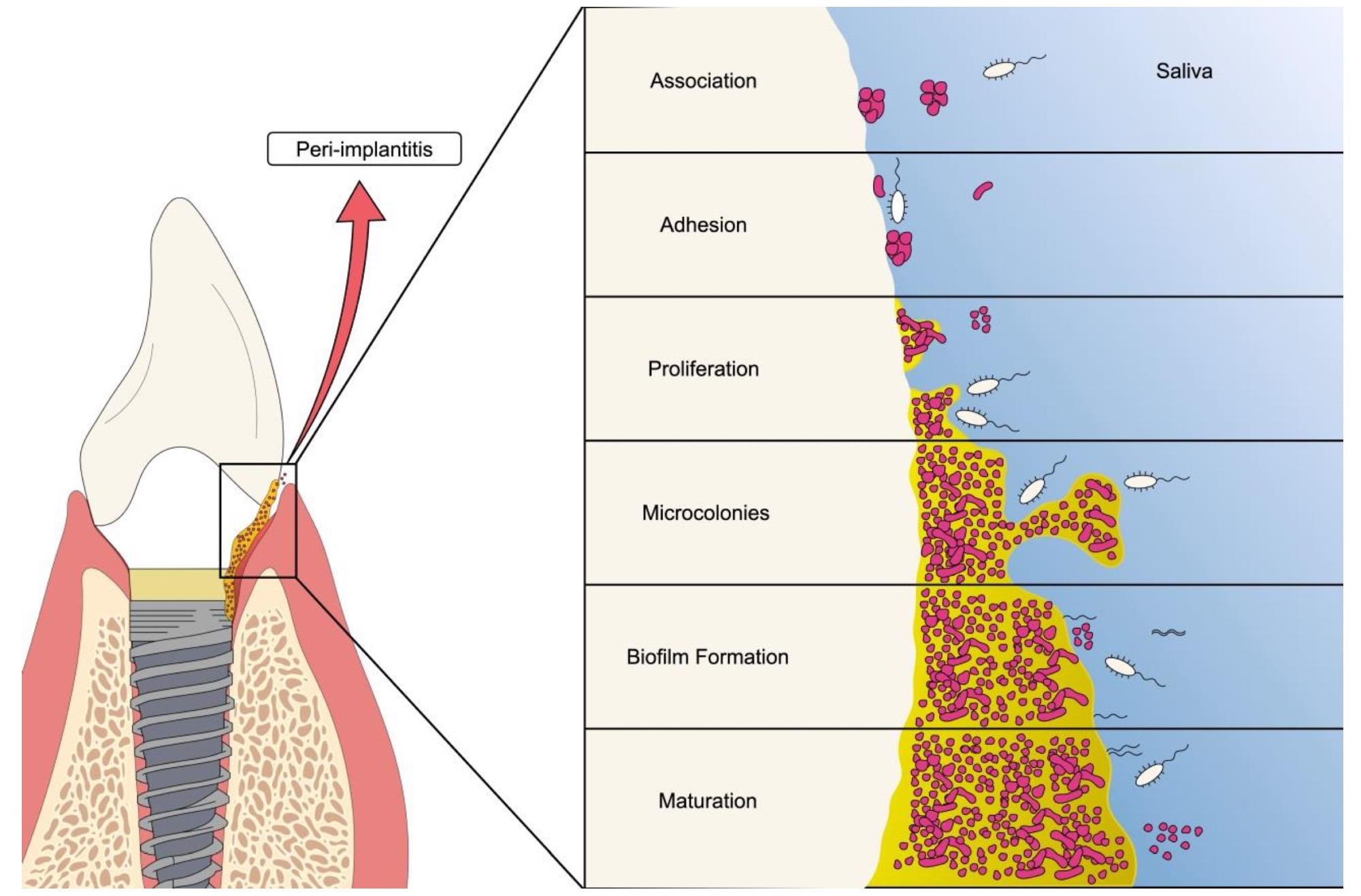
Schematic representation of oral biofilm formation on dental implants. The figure shows the different stages of bacterial biofilm formation ranging from adhesion to the establishment of the mature colony. Image Credit: Silva, R. C. S et al., Materials
The oxide TiO2 was present on the surface of the primary materials such as CpTi and Ti-6Al-4V used as dental implants, which allowed for high corrosion resistance and a clinical success rate of up to 99%. The α-β combination alloy i.e., Ti-6Al-4V, which was reported to be the most commonly used in dental applications, was made up of 4% vanadium and 6% aluminum and was extremely robust and corrosion-resistant.
When compared to smooth surfaces, nanoscale alterations and bioactivation of surfaces with biological molecules could promote quicker healing. It was also demonstrated in recent research that the incremental alterations in the implant, which were dependent on the microenvironment of insertion, could improve the implant's integration with soft and bone tissues and reduce the risk of infection and osseointegration failures.
Conclusions
In conclusion, this study elucidated that nanobiotechnological surface alterations in titanium dental implants increased the osseointegration process, which was found to be a critical factor in the development of better dental materials.
When compared to smooth surfaces, characteristics including chemical composition and shape were found to be promising for the production of biomimetic surfaces, which resulted in implants that promote faster and more efficient osseointegration. Nanostructured surfaces could provide a porosity topography that was similar to bone. Biomolecule coatings could promote osseointegration by promoting cell adhesion, proliferation, differentiation, and migration.
The authors mentioned that hybrid implants, with various types of alterations depending on the microenvironment of insertion, are future problems that may appear as novel materials for dental implant manufacture.
Disclaimer: The views expressed here are those of the author expressed in their private capacity and do not necessarily represent the views of AZoM.com Limited T/A AZoNetwork the owner and operator of this website. This disclaimer forms part of the Terms and conditions of use of this website.
Source:
Silva, R. C. S., Agrelli, A., Andrade, A. N., et al. Titanium Dental Implants: An Overview of Applied Nanobiotechnology to Improve Biocompatibility and Prevent Infections. Materials 15(9) 3131 (2022). https://www.mdpi.com/1996-1944/15/9/3150